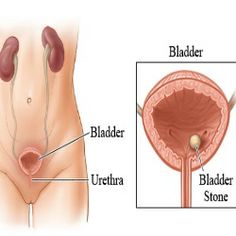
The bladder has a contraction phase for emptying and a storage phase that allows for storing urine. Sometimes problems with both functions contribute to OAB symptoms of frequency, urgency, getting up at night and incontinence. This is why sometimes the urologist will use two medicines to maximize treatment results. The articles below explain.
Do You Know the 2 Neural Pathways of OAB?
Sponsored by Astellas Pharma US, Inc.
What is overactive bladder?
Overactive bladder (OAB) is a clinical diagnosis characterized by a sudden, urgent need to urinate, with or without urine leakage, usually with daytime and nighttime (nocturia) frequency, in the absence of a urinary tract infection or other obvious pathology.1
Neurologic control of the bladder
As you may know, the urinary bladder has 2 primary functions: filling/storing urine during the storage phase, and rapidly expelling urine during the voiding (micturition) phase. The symptoms of OAB are usually associated with involuntary contractions of the detrusor muscle. This may result in urgency or urge incontinence.2,3
Neurotransmitters and the bladder
In the storage phase3:
-
- Norepinephrine released from sympathetic nerves interacts with β3‑adrenergic receptors
- Adenylate cyclase is activated, increasing intracellular cAMP levels
- Bladder smooth muscle relaxes
- M2/M3 receptors are the predominant muscarinic receptors found in the bladder. Binding of acetylcholine to M3 receptors on the detrusor muscle activates a signaling pathway that leads to bladder contraction and voiding. M3 receptors appear to be important for normal bladder contraction with M2 receptor activation serving a more prominent role in certain disease states (demonstrated in vitro)4-6
Do your OAB patients know what’s causing their symptoms?
Astellas is committed to helping your OAB patients better understand their symptoms.
Visit https://www.astellasresources.com/urology-resources for patient tools and helpful resources.
QUIZ
Which of the following is the correct signaling cascade?
- Sympathetic nerve → acetylcholine → β3‑adrenergic receptors → bladder relaxation
- Parasympathetic nerve → acetylcholine → muscarinic receptors → bladder contraction
- Parasympathetic nerve → norepinephrine → muscarinic receptors → bladder relaxation
- Sympathetic nerve → norepinephrine → β3‑adrenergic receptors → bladder contraction
Correct! The correct signaling cascade is Parasympathetic nerve → acetylcholine → muscarinic receptors → bladder contraction
Incorrect! The correct signaling cascade is Parasympathetic nerve → acetylcholine → muscarinic receptors → bladder contraction
References:
- Gormley EA, Lightner DJ, Burgio KL, et al. Diagnosis and Treatment of Overactive Bladder (Non-Neurogenic) in Adults: AUA/SUFU guideline. Linthicum, MD: American Urological Association Education and Research, Inc.; 2014:1-57.
- Andersson KE, Arner A. Urinary bladder contraction and relaxation: physiology and pathophysiology. Physiol Rev. 2004;84(3):935-986.
- Ouslander JG. Management of overactive bladder. N Engl J Med. 2004;350(8):786-799.
- Chess-Williams R, Chapple CR, Yamanishi T, Yasuda K, Sellers DJ. The minor population of M3-receptors mediate contraction of human detrusor muscle in vitro. J Auton Pharmacol. 2001;21(5-6):243-248.
- Yamaguchi O, Shishido K, Tamura K, Ogawa T, Fujimura T, Ohtsuka M. Evaluation of mRNAs encoding muscarinic receptor subtypes in human detrusor muscle. J Urol. 1996;156(3):1208-1213.
- Anderson KE. Pharmacology of lower urinary tract smooth muscles and penile erectile tissues. Pharmacol Rev. 1993;45(3):253-308.
In OAB: Targeting a Different Receptor Signaling Pathway in the Bladder
Sponsored by Astellas Pharma US, Inc.
Click here to see the full Prescribing Information for Myrbetriq® (mirabegron).
Myrbetriq® (mirabegron)—targeting a different receptor signaling pathway in the bladder
Myrbetriq is the first and only FDA-approved β3‑adrenergic agonist for the treatment of overactive bladder (OAB) with symptoms of urge urinary incontinence, urgency, and urinary frequency.1
Bladder storage and voiding in OAB: Storage makes up the majority of the micturition cycle
|
Bladder storage2,3 |
Bladder voiding2,3 |
| Primary regulator |
Sympathetic nervous system |
Parasympathetic nervous system |
| Mediating neurotransmitter |
Norepinephrine |
Acetylcholine |
The parasympathetic and sympathetic autonomic nervous systems control the micturition cycle2,3
- Storage is regulated primarily by the neurotransmitter norepinephrine, which is released by sympathetic nerves
- Norepinephrine binds to and activates β3‑adrenergic receptors (ARs) on the bladder’s detrusor muscle
- The activated β3‑ARs relax the detrusor muscle, allowing the bladder to store more urine
- The β‑ARs belong to a family of G-protein–coupled receptors, which are involved with cellular signaling throughout the body and are made up of 3 subtypes (β1, β2, β3)4,5
- All 3 β‑AR subtypes are expressed in the human bladder, but β3-messenger RNA (mRNA) predominates, accounting for 97% of β‑AR mRNA in the bladder6
- The β1‑AR and β2‑AR subtypes make up 1.5% and 1.4% of the total β‑AR mRNA, respectively
Mirabegron is not an antimuscarinic agent. It targets a different receptor signaling pathway—the β3‑AR pathway
- OAB is characterized by involuntary contraction of the detrusor muscle during the storage phase7
- Mirabegron relaxes the detrusor smooth muscle during the storage phase of the urinary bladder fill-void cycle by activation of the β3‑AR1
- Mirabegron is an agonist of the human β3‑AR as demonstrated by in vitro laboratory experiments using the cloned human β3‑AR1
- Although mirabegron showed very low intrinsic activity for cloned human β1‑AR and β2‑AR, results in humans indicate that β1‑AR stimulation occurred at a mirabegron dose of 200 mg1
INDICATIONS AND USAGE
Myrbetriq® (mirabegron) is a beta‑3 adrenergic agonist indicated for the treatment of overactive bladder (OAB) with symptoms of urge urinary incontinence, urgency, and urinary frequency.
IMPORTANT SAFETY INFORMATION
Myrbetriq is contraindicated in patients who have known hypersensitivity reactions to mirabegron or any component of the tablet.
Myrbetriq can increase blood pressure. Periodic blood pressure determinations are recommended, especially in hypertensive patients. Myrbetriq is not recommended for use in severe uncontrolled hypertensive patients (defined as systolic blood pressure ≥ 180 mm Hg and/or diastolic blood pressure ≥ 110 mm Hg).
Urinary retention in patients with bladder outlet obstruction (BOO) and in patients taking antimuscarinic medications for the treatment of OAB has been reported in postmarketing experience in patients taking mirabegron. A controlled clinical safety study in patients with BOO did not demonstrate increased urinary retention in Myrbetriq patients; however, Myrbetriq should be administered with caution to patients with clinically significant BOO. Myrbetriq should also be administered with caution to patients taking antimuscarinic medications for the treatment of OAB.
Angioedema of the face, lips, tongue and/or larynx has been reported with Myrbetriq. In some cases angioedema occurred after the first dose. Cases of angioedema have been reported to occur hours after the first dose or after multiple doses. Angioedema associated with upper airway swelling may be life threatening. If involvement of the tongue, hypopharynx, or larynx occurs, promptly discontinue Myrbetriq and initiate appropriate therapy and/or measures necessary to ensure a patent airway.
Since Myrbetriq is a moderate CYP2D6 inhibitor, the systemic exposure to CYP2D6 substrates such as metoprolol and desipramine is increased when co-administered with Myrbetriq. Therefore, appropriate monitoring and dose adjustment may be necessary, especially with narrow therapeutic index drugs metabolized by CYP2D6, such as thioridazine, flecainide, and propafenone.
In clinical trials, the most commonly reported adverse reactions (> 2% and > placebo) for Myrbetriq 25 mg and 50 mg versus placebo, respectively, were hypertension (11.3%, 7.5% vs 7.6%), nasopharyngitis (3.5%, 3.9% vs 2.5%), urinary tract infection (4.2%, 2.9% vs 1.8%), and headache (2.1%, 3.2% vs 3.0%).
In postmarketing experience, the following events have also occurred: constipation, diarrhea, and dizziness.
Click here to see the full Prescribing Information for Myrbetriq® (mirabegron).
Is Myrbetriq right for your OAB patients with symptoms of urge urinary incontinence, urgency, and urinary frequency?
Visit www.MyrbetriqHCP.com to learn more.